We’ve sent over 1,000 letters – let’s keep the pressure on UnitedHealthcare

Keep the momentum going – send a letter, share with your patients and use social media.
We’ve sent 880+ letters to United’s CEO, and we’re not done!

Act now and tell United not to implement new prior auth requirements on June 1.
New resources to tell UnitedHealthcare “no” on prior auth

Use our pre-written tweets or letter to tell United to stop new prior auth requirements from going into effect June 1.
Tell UnitedHealthcare to stop new prior authorization requirements

Patients don’t need more obstacles to care and you don’t need more red tape.
AGA takes CRC month to Capitol Hill

Member highlights from a busy month of advocacy events in support of Colorectal Cancer Awareness Month.
Introducing AGA’s top advocacy priorities for 2023

Our focus includes prior authorization reform and Medicare reimbursement.
What the omnibus bill means for GI

Funding bill includes telehealth extension, increased NIH funding and AGA report language on IBD.
AGA members advocate for GI during Alliance of Specialty Medicine Fly-In
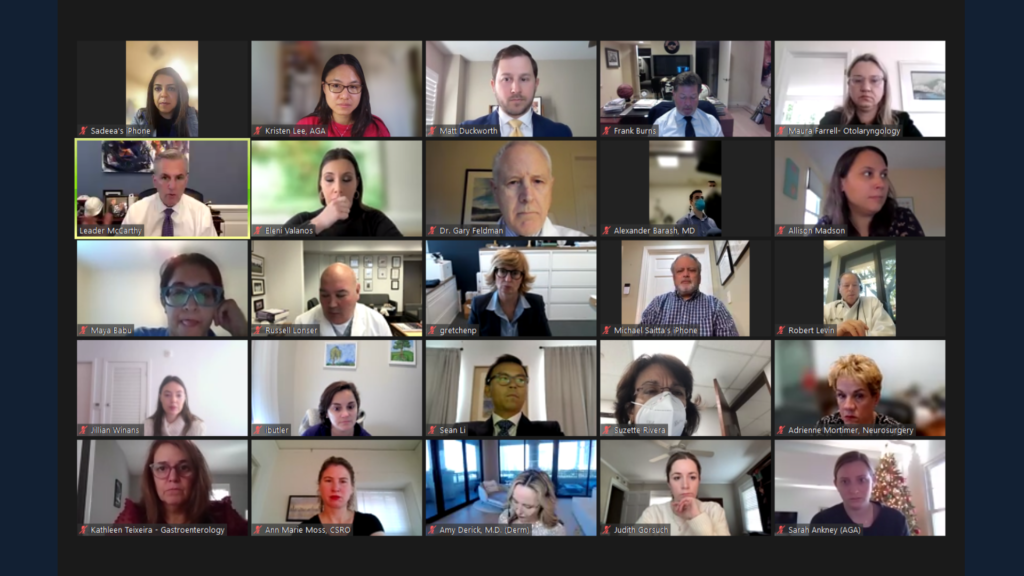
Six members represented AGA during the meetings and called on lawmakers to act on key priorities, including impending Medicare cuts.
GI payments face steep cuts unless Congress acts

GIs who treat Medicare patients will face cuts up to 8.5 percent in the new year unless Congress intervenes.
What the election results mean for GI

The majorities in both chambers are razor thin. We are pushing to prevent Medicare cuts and reform prior auth.











