Surgical interventions and the use of device-aided therapy for the treatment of fecal incontinence and defecatory disorders
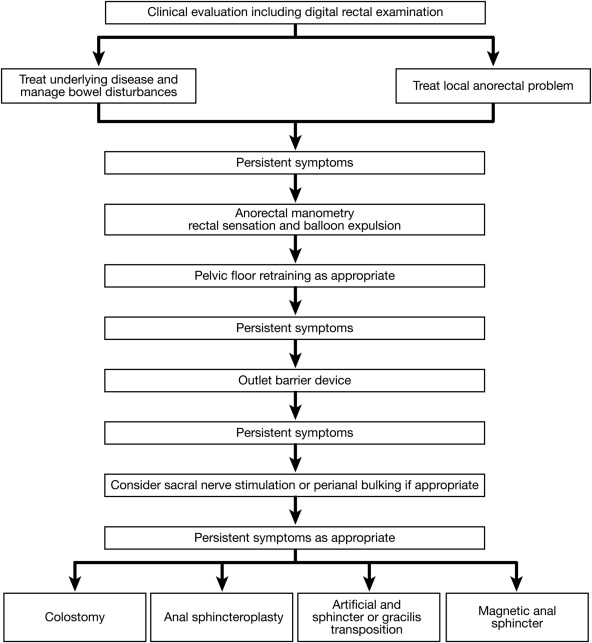
How to best use surgical interventions and device-aided therapy for managing fecal incontinence (FI) and defecatory disorders.
Incorporating psychogastroenterology into management of digestive disorders
How to integrate psychological care and make an effective referral for brain-gut psychotherapy in routine practice.
Functional gastrointestinal symptoms in patients with inflammatory bowel disease (IBD)
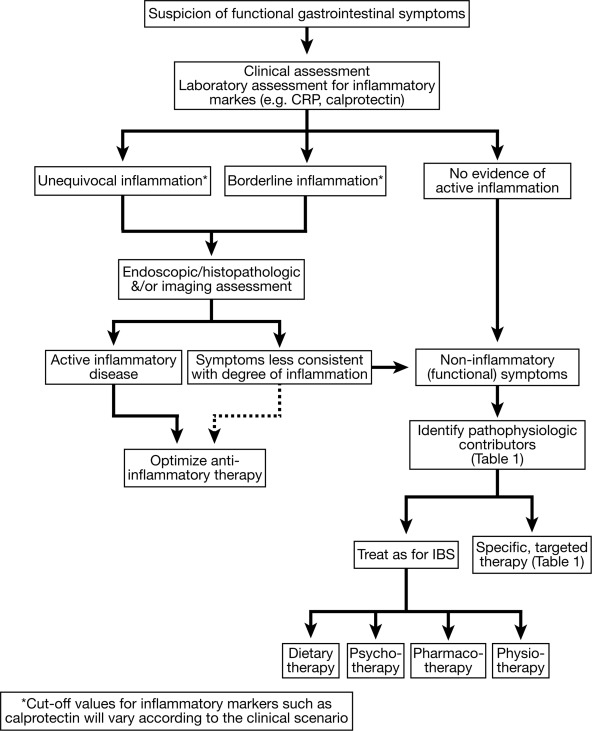
Key principles in the diagnosis and management of functional GI symptoms in patients with inflammatory bowel disease (IBD).
Switching between biologics and biosimilars in inflammatory bowel disease (IBD)
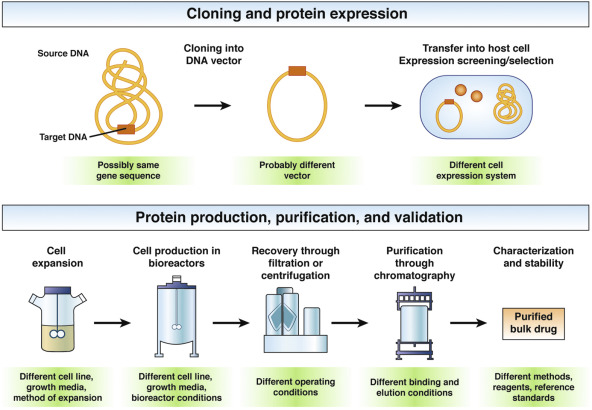
Get an overview of biosimilars, their manufacturing process, the FDA approval process, and the data available describing their safety and efficacy for Crohn’s disease and ulcerative colitis.
Medical management of opioid-induced constipation
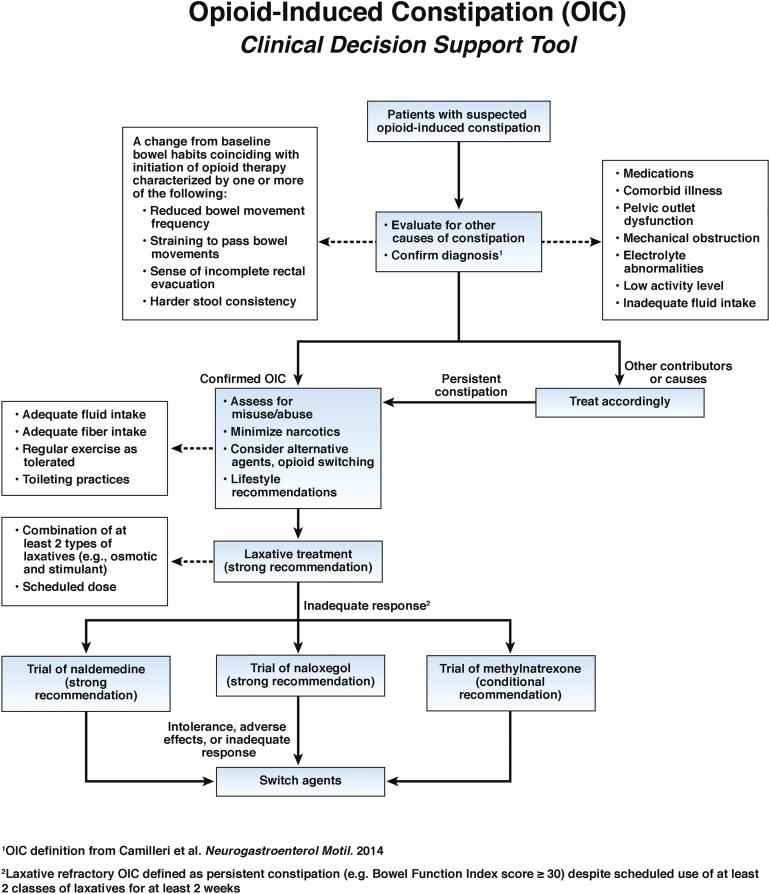
Guidance to select the right treatment for your patients experiencing opioid-induced constipation (OIC).
Management of mild-to-moderate ulcerative colitis
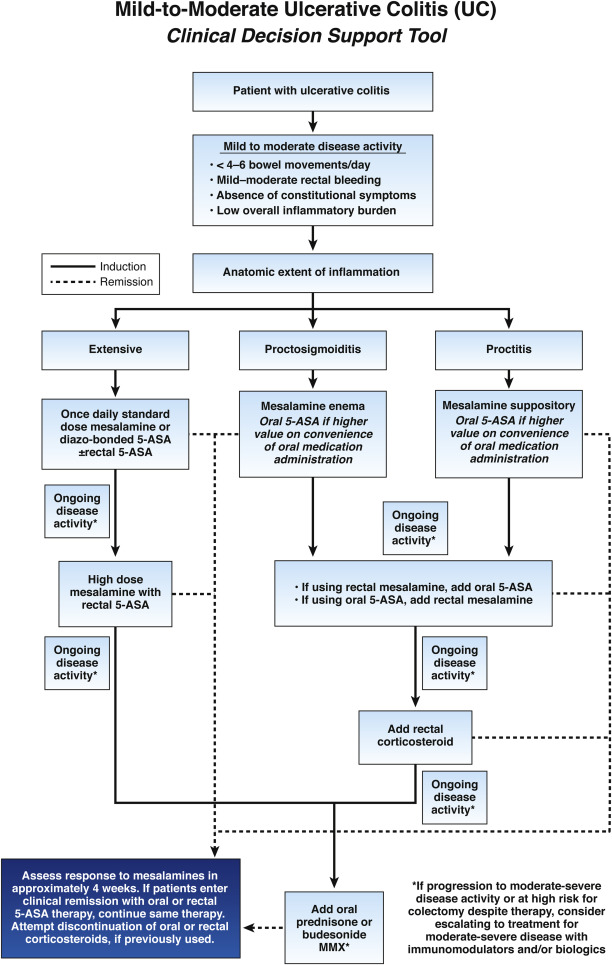
Best practices for managing patients with mild-to-moderate ulcerative colitis (UC), focusing on use of both oral and topical 5-aminosalicylates (5-ASA) medications, rectal corticosteroids and oral budesonide.
Diagnosis and monitoring of celiac disease: changing utility of serology and histologic measures
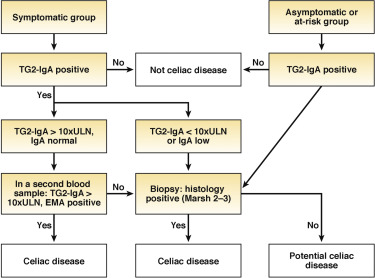
Best practices for diagnosing and managing celiac disease in adults as well as in children and adolescents.
Inflammatory bowel disease (IBD) in pregnancy clinical care pathway
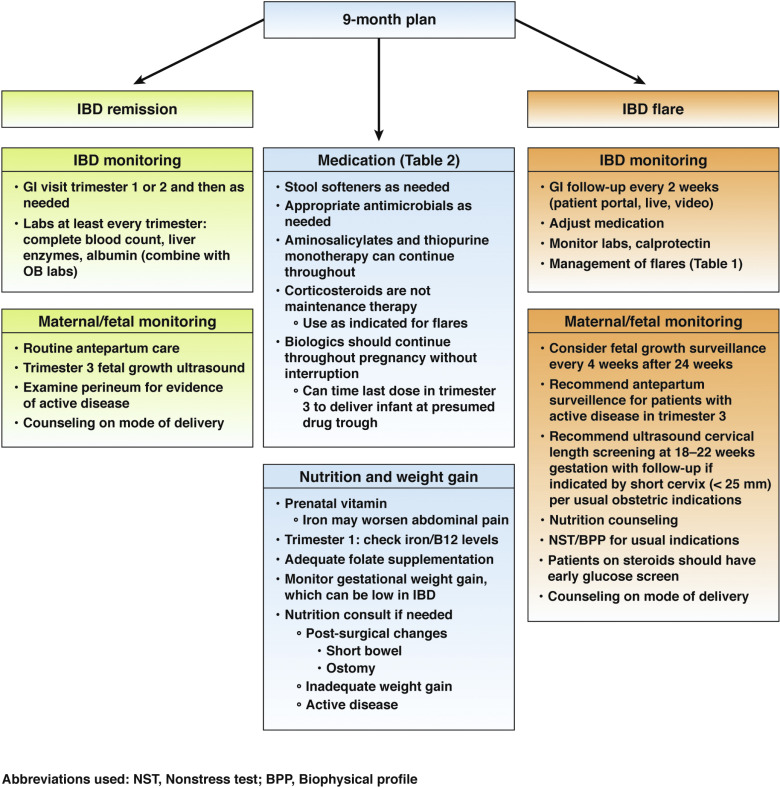
An outline of the entire care process — from preconception counseling through the postpartum phase — for your patients with Crohn’s disease and ulcerative colitis in their reproductive years.
Laboratory evaluation of functional diarrhea and diarrhea-predominant irritable bowel syndrome in adults (IBS-D)
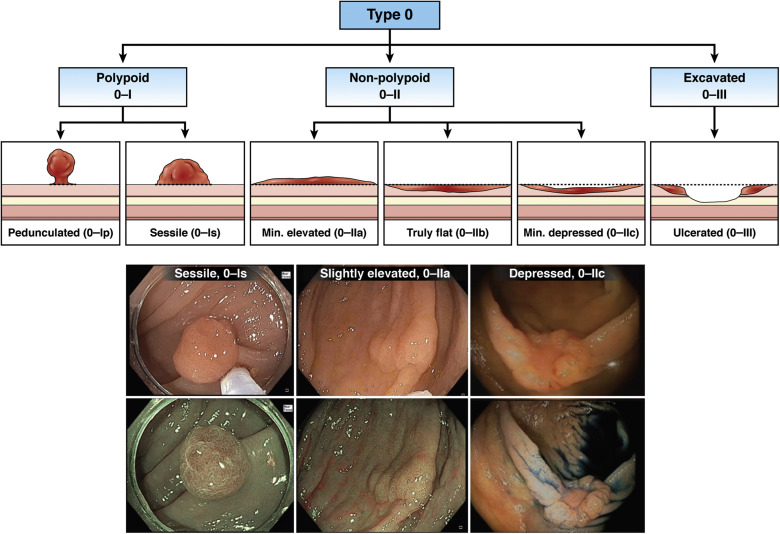
How to choose the best laboratory tests to identify functional diarrhea and diarrhea-predominant irritable bowel syndrome (IBS-D) in adults and exclude other diagnoses. These guidelines apply to the evaluation of the immunocompetent patient with “watery” diarrhea of at least 4 weeks duration.
Management of moderate-to-severe ulcerative colitis
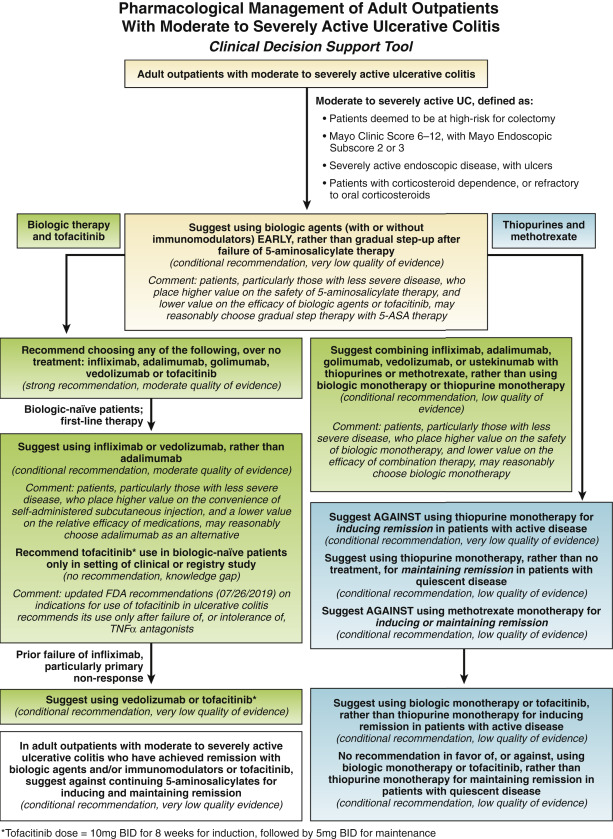
How to manage adult outpatients with moderate-to-severe ulcerative colitis (UC) as well as adult hospitalized patients with acute severe ulcerative colitis (ASUC). The guideline focuses on immunomodulators, biologics, and small molecules to bring on and maintain remission for patients with moderate to severe UC and to decrease the risk of colectomy.











