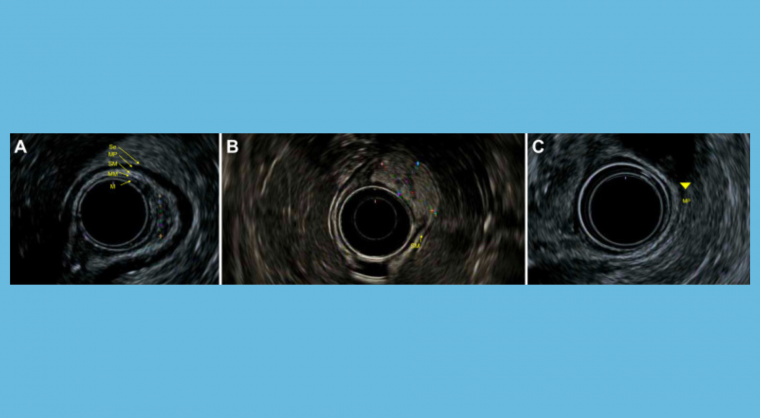
AGA has released a new Clinical Practice Update providing best practice advice on how to manage subepithelial lesions (SEL) during routine endoscopies.
Best practice advice
- Forceps bite-on-bite or deep-well biopsies or tunnel biopsies can sometimes establish a pathologic diagnosis of SEL.
- Endoscopic ultrasound (EUS) is the modality of choice to evaluate indeterminate SEL of the GI track and/or if nondiagnostic tissue by forceps biopsies.
- SEL arising from the submucosa can be sampled using tunnel biopsies (or deep-well biopsies), EUS guided fine-needle aspiration (FNA), EUS guided fine-needle biopsy (FNB), or advanced endoscopic techniques (unroofing or endoscopic submucosal resection).
- SEL arising from muscularis propria should be sampled (preferably using FNB or FNA) to determine whether the lesion is a GIST or leiomyoma. Structural assessment and staining will allow differentiation of mesenchymal tumors and assessing their malignant potential.
- Endoscopic resection techniques have been described for removal of SEL and should be limited to endoscopists skilled in advanced tissue resection techniques.
- Management of each SEL depends on the size of the lesion, histopathology, their malignant potential and presence of symptoms.
- SEL that have an endoscopic appearance consistent with a lipoma or pancreatic rest and normal mucosal biopsies do not need further evaluation or surveillance.
- For SEL arising from muscularis propria that are less than 2 cm in size, surveillance using EUS should be considered.
- Gastric GIST larger than 2 cm should be considered for resection.
- Subepithelial lesions that are ulcerated, bleeding, or causing symptoms should be considered for resection.
Hear directly from author Dr. Kaveh Sharzehi on his key takeaways from this Clinical Practice Update: