Modeling studies and expert consensus published this week in Gastroenterology and Clinical Gastroenterology and Hepatology shed new light on the promise and peril of liquid biopsy (blood tests) for CRC screening that are currently in development.


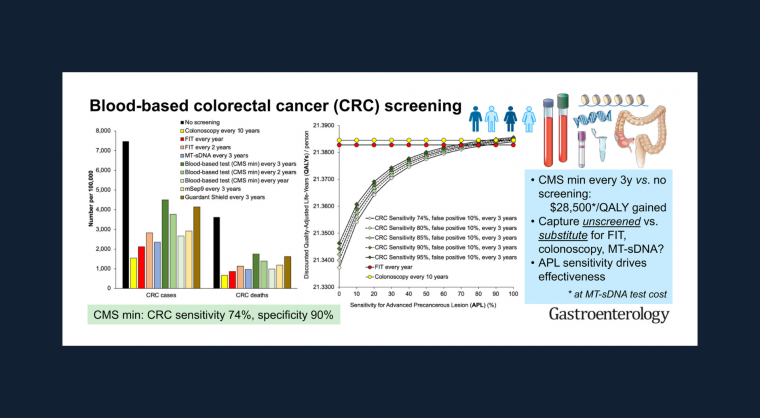
An AGA expert panel set out to estimate the effects of a new blood-based CRC screening test on an average-risk population aged 45-75, assuming the test met minimal CMS criteria for CRC sensitivity (74%) and specificity (90%). The aim was to define properties of a successful CRC screening blood test and compare possible outcomes with the established strategies of FIT, MT-sDNA tests (Cologuard) and colonoscopies.
Here are the key conclusions found:
- A blood test for CRC that meets minimal CMS criteria for sensitivity and performed every three years would likely result in better outcomes than no screening.
- A blood test for CRC offers a simple process that could encourage more people to participate in screening. Patients who may have declined colonoscopy should understand the need for a colonoscopy if findings are abnormal.
- Because blood tests for CRC are predicted to be less effective and more costly than currently established screening programs, they cannot be recommended to replace established effective screening methods.
- Although blood tests would improve outcomes in currently unscreened people, substituting blood tests for a currently effective test would worsen patient outcomes and increase cost.
- Potential benchmarks that industry might use to assess an effective blood test for CRC going forward would be sensitivity for stage I-III CRC of >90%, with sensitivity for advanced adenomas of > 40-50%.
The expert panel analyzed modeling performed by two independent groups. Those studies are now available in Gastroenterology:
- Effectiveness and Cost-Effectiveness of Colorectal Cancer Screening With a Blood Test That Meets the Centers for Medicare & Medicaid Services Coverage Decision
- Comparative Effectiveness and Cost-Effectiveness of Colorectal Cancer Screening With Blood-Based Biomarkers (Liquid Biopsy) vs Fecal Tests or Colonoscopy