AGA has released a new Clinical Practice Update providing best practice advice on clinical management of suspected acute kidney injury (AKI) in patients with cirrhosis.
Key takeaways:
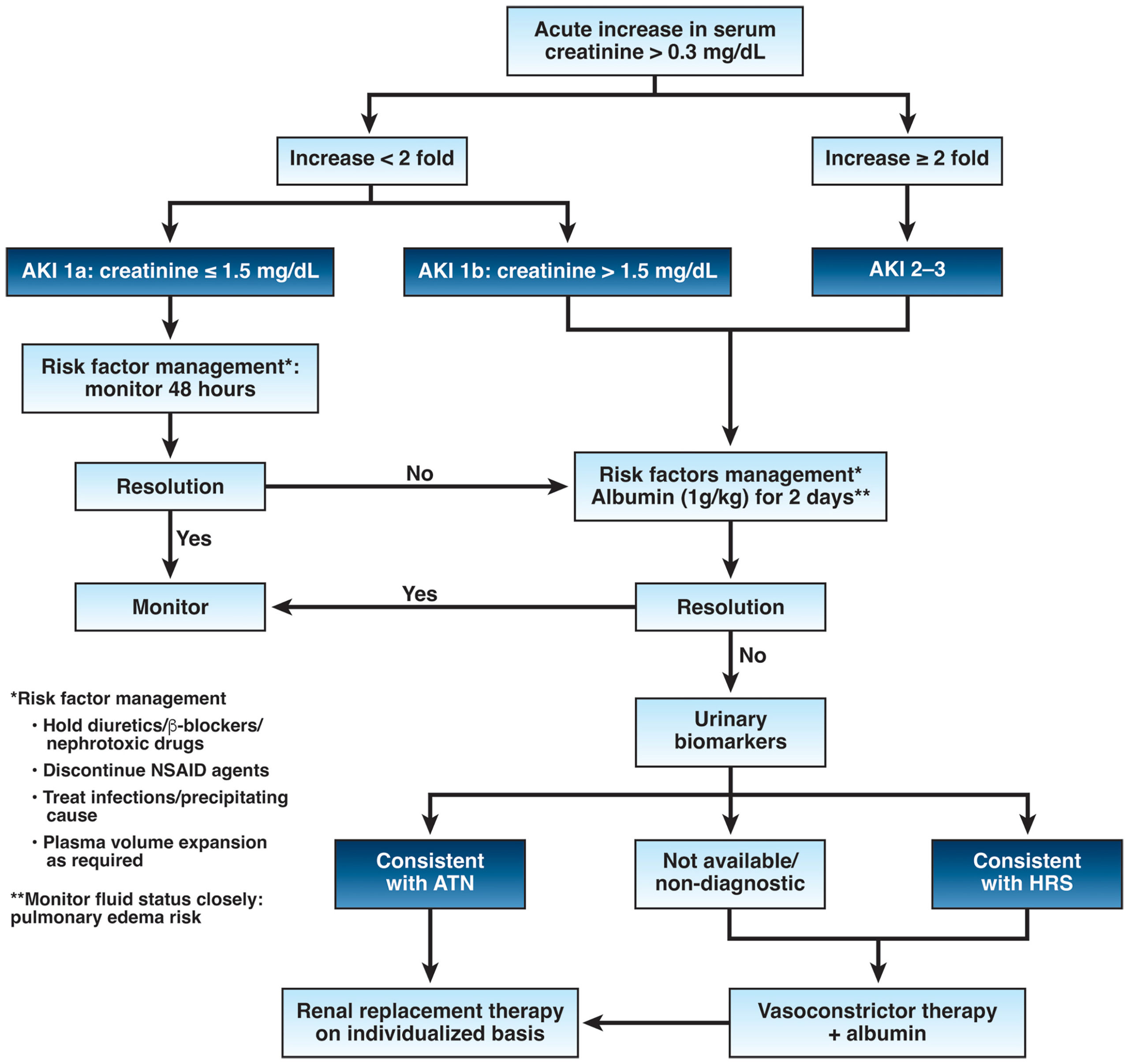
- AKI should be diagnosed when the serum creatinine increases by ≥ 0.3 mg/dl within 48 hours, or ≥50 percent from baseline or when the urine output is reduced below 0.5ml/kg/hr for > 6 hours.
- The specific type of AKI should be identified through a careful history; physical examination; blood biochemistry; urine microscopic examination; urine chemistry (Na+ and urea) and selected urinary biomarkers; and renal ultrasound.
- When the serum creatinine remains higher than twice the baseline value despite withdrawal of diuretics and albumin infusion, treatment of HRS-AKI should be initiated with albumin at a dose of 1 g/kg intravenously on day 1 followed by 20-40 g daily along with vasoactive agents (terlipressin or norepinephrine, depending on institutional preferences) and continued either until 24 hours following the return of the serum creatinine level to ≤ within 0.3mg/dl of baseline for two consecutive days or for a total of 14 days of therapy.
Clinical decision support tool
Watch author Dr. Joseph Ahn share his key takeaways from this Clinical Practice Update.
Read all 14 best practice statements in AGA Clinical Practice Update on the Evaluation and Management of Acute Kidney Injury in Patients With Cirrhosis: Expert Review published in the December issue of Clinical Gastroenterology and Hepatology.