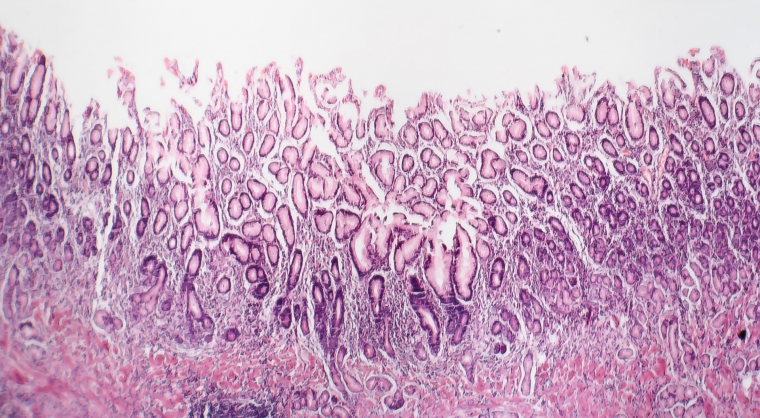
AGA’s new Clinical Practice Update provides 12 best practice advice statements for the diagnosis and management of atrophic gastritis, with a primary focus on atrophic gastritis due to chronic Helicobacter pylori infection.
Best practice advice
- Atrophic gastritis is defined as the loss of gastric glands, with or without metaplasia, in the setting of chronic inflammation mainly due to H. pylori infection or autoimmunity. Regardless of the etiology, the diagnosis of atrophic gastritis should be confirmed by histopathology.
- Be aware that the presence of intestinal metaplasia on gastric histology almost invariably implies the diagnosis of atrophic gastritis. We advise a coordinated effort between gastroenterologists and pathologists to improve the consistency of documenting the extent and severity of atrophic gastritis, particularly if marked atrophy is present.
- Recognize typical endoscopic subtle features of atrophic gastritis, which include pale appearance of gastric mucosa, increased visibility of vasculature due to thinning of the gastric mucosa, and loss of gastric folds, and, if with concomitant intestinal metaplasia, light blue crests and white opaque fields. Due to the subtlety, techniques to optimize evaluation of the gastric mucosa should be performed.
- When endoscopic features of atrophic gastritis are present, assess the extent endoscopically and obtain biopsies from the suspected atrophic/metaplastic areas for histopathological confirmation and risk stratification; at a minimum, biopsies from the body and antrum/incisura should be obtained and placed in separately labeled jars. Targeted biopsies should additionally be obtained from any other mucosal abnormalities.