Through the end of the year, we’re bringing back some of the best articles from the AGA Journals blog, Digest This. Learn more about the significance of polyp size in this article originally published in June 2010.
Computed tomography colonography (CTC) is a useful tool for colon cancer screening. The challenge, however, is determining which lesions are most dangerous — should some be treated aggressively and others just monitored or ignored? Does size matter?
In the July issue of Clinical Gastroenterology and Hepatology, Perry Pickhardt et al. assessed the rates of cancer and high-grade dysplasia that developed among more than 5,000 individuals who were screened by CTC; those found to have colon polyps were followed for 52 months. During this time, none of the patients that had small polyps (6-9 mm) developed malignancy and only 0.4 percent developed low-grade dysplasia. Small polyps therefore appear to be harmless, although these values are lower than those from previous studies. The authors point out that older studies were performed in symptomatic, high-risk cohorts and that this study more accurately reflects the general population.
Larger polyps, however, pose a greater threat. Pickhardt et al. found that that cancer incidence increased with polyp size — 91 percent of all advanced adenomas and 100 percent of cancer cases were from individuals with lesions of 10 mm or larger. The authors therefore propose a less-aggressive management strategy for people with small polyps and 3 cm as a ‘point-of-no-return’ in the progression of a benign colonic lesion to a malignancy. Some researchers have proposed 15-20 mm as the threshold for polypectomy, which is costly and can have complications.
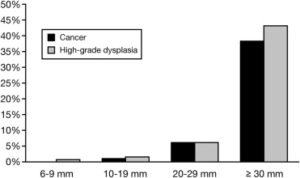
Bar graph of the frequency of cancer and high-grade dysplasia according to polyp size shows the critical importance of lesion size for predicting clinical relevance. Of note, high-grade dysplasia and malignancy are rare among polyps less than 20 mm in size.
A firm cut-off size for polyps is difficult to establish because rates of adenoma growth and dysplastic progression are not linear, which might account for the fact that the patients in Pickhardt’s study had more polyps >30 mm than in the 20-29 mm range. What if a patient has numerous small lesions — are they at greater risk for cancer than a person with fewer polyps?
Cost-benefit studies are needed; the cost of identifying early-stage cancers is high and appropriate surveillance intervals for large lesions might be too short to be cost effective.
While AGA maintains that colonoscopy is the gold standard for the detection and prevention of colorectal cancer (CRC), it does acknowledge that CTC, if performed properly, is a valuable technology that can increase screening rates and thus reduce the incidence of mortality from CRC.
Read the full article online in Clinical Gastroenterology and Hepatology.

Kristine Novak, MD
Dr. Novak is a science writer and editor based in San Francisco. She has extensive experience covering gastroenterology, hepatology, immunology, oncology, clinical and biotechnology research discoveries.













