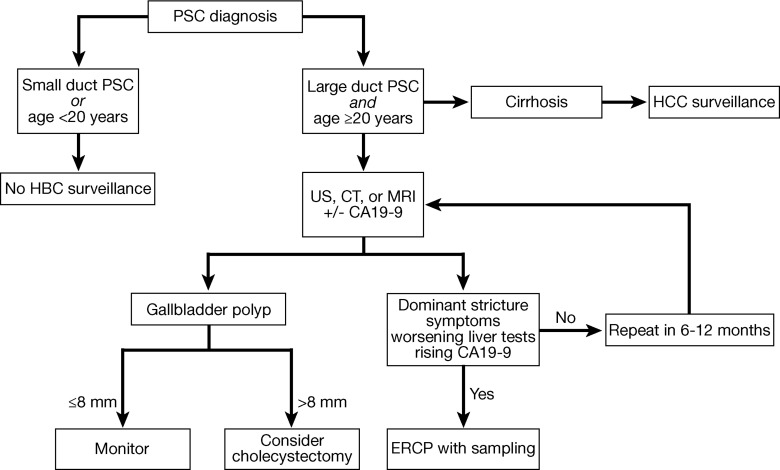
1. Surveillance for cholangiocarcinoma and gallbladder cancer should be considered in all adult patients with primary sclerosing cholangitis (PSC) regardless of disease stage, especially in the first year after diagnosis and in patients with ulcerative colitis and those diagnosed at an older age.
2. Surveillance for cholangiocarcinoma and gallbladder cancer should include imaging by ultrasound, computed tomography (CT), or magnetic resonance imaging (MRI), with or without serum carbohydrate antigen 19-9, every 6 to 12 months
3. Endoscopic retrograde cholangiopancreatography (ERCP) with brush cytology should not be used routinely for surveillance of cholangiocarcinomas in PSC.
4. Cholangiocarcinomas should be investigated by ERCP with brush cytology with or without fluorescence in situ hybridization analysis and/or cholangioscopy in PSC patients with worsening clinical symptoms, worsening cholestasis or a dominant stricture.
5. Fine-needle aspiration of perihilar biliary strictures should be used with caution in PSC patients considered to be liver transplant candidates because of concerns for tumor seeding if the lesion is a cholangiocarcinoma.
6. Surveillance for cholangiocarcinoma should not be performed in PSC patients with small-duct PSCs or those younger than age 20.
7. The decision to perform a cholecystectomy in PSC patients with a gallbladder polyp should be based on the size and growth of the polyp, as well as the clinical status of the patient, with the knowledge of the increased risk of gallbladder cancer in polyps greater than 8 mm.
8. Surveillance for hepatocellular carcinoma in PSC patients with cirrhosis should include ultrasound, CT or MRI, with or without α-fetoprotein every 6 months.