This week, the president announced an expansion of telehealth benefits for Medicare beneficiaries during the COVID-19 public health emergency to allow clinicians to bill telehealth services immediately for dates of service starting March 6, 2020. Telehealth will be paid under the Medicare Physician Fee Schedule at the same amount as in-person services and HIPAA rules have been temporarily waived to allow physicians to provide telehealth services through remote, non-public facing communications technologies, like FaceTime and Skype. Some commercial payors are choosing to adopt all or part of these changes.
Our AGA member experts have developed a telehealth guide to help you understand and implement the changes. It includes:
- A brief overview of the changes
- Answers to frequently asked questions
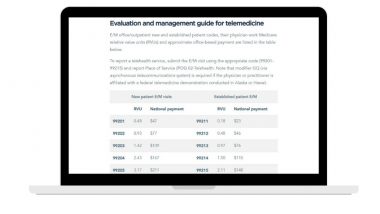
- Telehealth, virtual check-in, and e-consultation codes with guidance on use
- Online COVID-19 telehealth coverage and coding resources
The situation is evolving rapidly and we will update the telehealth guide to reflect any updates or changes to Medicare guidance and commercial payor adoption. We are also working with our sister societies on a joint coding guide for telehealth and e-visits which should be available soon.