What is ulcerative colitis?
Ulcerative colitis is a type of IBD.
There are two main types of inflammatory bowel diseases — ulcerative colitis and Crohn’s disease. Ulcerative colitis is more common worldwide than Crohn’s disease.
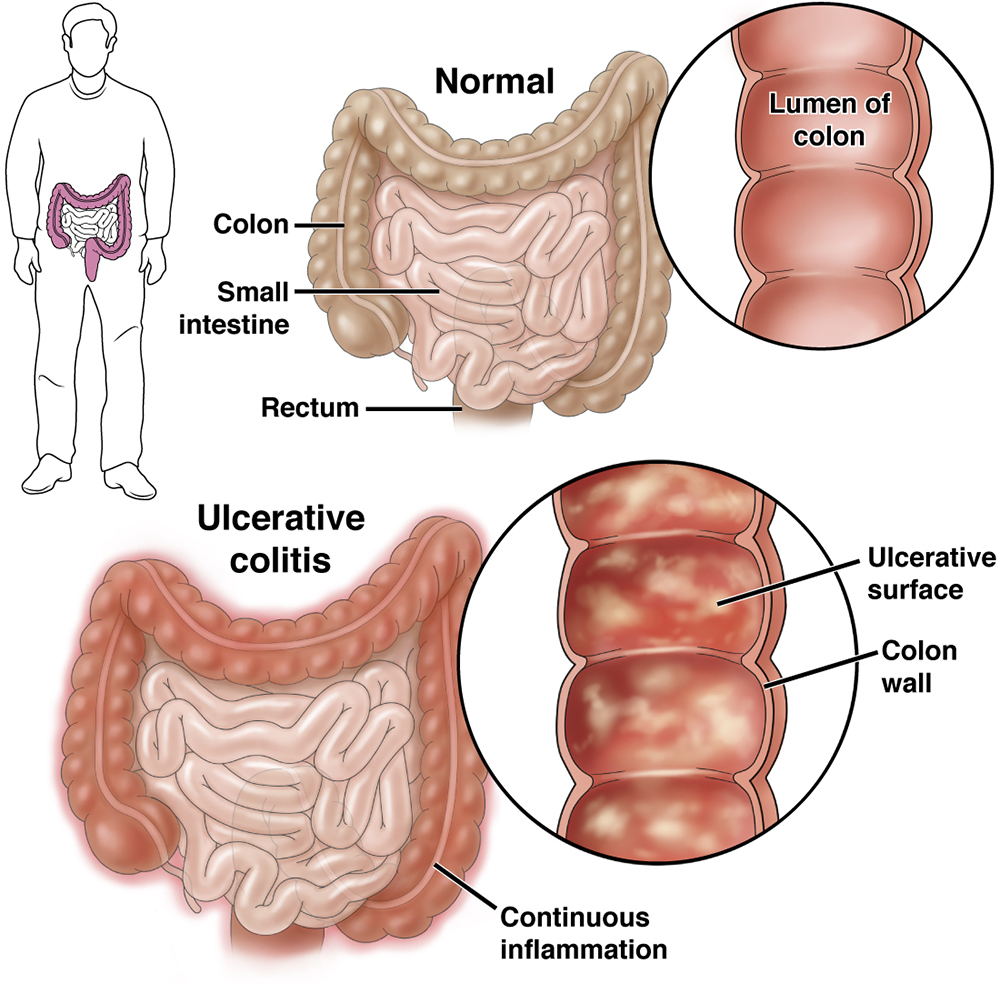
It causes inflammation (swelling) and sores (called ulcers) in the large intestine (colon and rectum) and may affect part or all of the large intestine.
Ulcerative colitis can happen at any age, but it is more likely to develop in people between the ages of 15 and 30, or older than 60 years of age.
Ulcerative colitis needs to be diagnosed by a health care provider. While there are no cures, there are treatments.
Terminology
Ulcerative colitis may start slowly and get worse for many weeks. It can have times of remission (time when your symptoms get better) or mildly, moderately or severely active. It can be described as fulminant, which means that it is severely active and not responding to therapy.
No blood or urgency and normal bowel function.
Fewer than four stools per day (with or without blood) without other symptoms and normal inflammatory markers.
Four or more bloody stools per day with minimal signs of other symptoms in the body.
More than six bloody stools per day with signs of systemic effects such as:
- Fevers.
- Abnormally rapid heart rate.
- Anemia (red blood cell deficiency).
More than 10 bloody bowel movements per day and may have other symptoms, including abdominal swelling or the need for blood transfusions.
Symptoms of ulcerative colitis
Most symptoms of ulcerative colitis relate to bowel movements.
The symptoms of ulcerative colitis can vary from person to person, based on where the disease is in the body and how bad the inflammation is.
Most common symptoms:
- Diarrhea (loose stool), which is often the first symptom.
- Blood in the stool.
- Urgency, or immediate need, to go to the bathroom.
- Increased number of bowel movements.
- Belly pain and cramping.
Ulcerative colitis can cause symptoms throughout your body.
You might have weight loss or other symptoms that affect the entire body. The inflammation of ulcerative colitis can also affect your joints or skin, leading to painful joints and skin rashes. During a flare-up, symptoms may go beyond those that affect the digestive system, including:
- Rashes or patches of red, swollen skin.
- Painful or swollen joints.
- Mouth ulcers.
- Red, irritated eyes.
Keep of track of any symptoms, how often you have them, and how bad they are to talk about with your health care provider.
Getting tested for ulcerative colitis
There are many tests your gastroenterologist can do to find out if you have ulcerative colitis. First, he or she will take your past health and family health info, listen to your symptoms, and do an exam to feel and listen to your belly. No one test makes the diagnosis, but testing is used to confirm the gastroenterologist’s clinical suspicion that ulcerative colitis is causing symptoms.
Ulcerative colitis is diagnosed by the presence of the common symptoms and endoscopic and biopsy (small tissue sample) findings of long-term inflammation in the large intestine.
Talk to your doctor about which test is best for you. Your doctor will tell you how to get ready for your test for ulcerative colitis.
Your doctor will look for anemia (low iron in your blood, which can make you feel weak and tired), caused by bleeding.
Blood tests can show signs of inflammation or infection somewhere in the body, like a high white blood cell count and other markers of inflammation.
Blood tests can be done at your doctor’s office or in a lab.
Stool tests are done to make sure there aren’t other gastrointestinal health problems, such as infection, causing symptoms.
Your doctor will give you a special holder for the stool, which is then returned to your doctor or a lab.
The below tests are done in your doctor’s office, an outpatient center or a hospital. These tests can be used to find ulcerative colitis or to rule out other health issues, such as Crohn’s disease, irritable bowel syndrome (IBS), diverticulitis or cancer.
You will be given medicine to make you feel relaxed and sleepy during this test.
A colonoscopy involves looking at the colon from inside the body using a long, thin (about the width of your little finger), flexible tube with a tiny camera on the end, through which the doctor can view your whole colon and rectum for inflammation, swollen tissue, ulcers or polyps (mushroom-like or flat growths on the inside wall of the colon or rectum).
If the doctor thinks it might be ulcerative colitis, he or she will also do a biopsy (taking a small piece of tissue to look at under the microscope) during the colonoscopy. This is not something you will be able to feel.
You might feel some pressure during the exam and there may be some cramping afterward, but you most likely will not feel a thing during this test.
You will need to “prep” before this test to clean out your bowel so your doctor can see clearly. Follow the instructions given to you by your doctor to do this.
Since you will be given medicine to make you sleepy, you will need someone to take you home and you won’t be able to go to work that day. The next day, most people go back their usual activities. Learn more about colonoscopy and how to prepare.
This test can be done in a doctor’s office and does not need anesthesia or sedation (medicine that makes you sleepy).
Sigmoidoscopy is a test during which a doctor uses a short, thin (about the width of your little finger), flexible tube with a tiny camera on the end to check the rectum and the lower end of the colon for polyps and cancer. Only the final two feet of the colon’s six feet are examined.
Introduction of the flexible tube may be somewhat uncomfortable, and some cramping may happen during the test.
You will need to take a couple of cleansing enemas before the test and/or a gentle oral prep.
You may be given medicine to make you relaxed and sleepy during this test.
The doctor may take a biopsy (a small piece of tissue to look at under a microscope). This is done during the test and is not something you will be able to feel. If a biopsy is done, you may see some traces of blood in your stool for a few days after the test. It will not impact your recovery.
After the test, there may be some mild belly-gas pains.
Treatment for ulcerative colitis
While there is no cure for ulcerative colitis, there are many options to help treat it.
The goals of treatment are to:
- Control inflammation, or swelling.
- Ease symptoms, like pain, diarrhea (loose stool) and bleeding.
- Fix nutrition deficiencies, if needed.
Treatment will depend on the severity of the disease, past complications and response to earlier treatments. Remember, everyone experiences symptoms of ulcerative colitis differently. If one treatment doesn’t work as well, there are other options. Just be sure to be in touch with your gastroenterologist often.
Treatment options for ulcerative colitis involve medications, surgery or a combination.
Medications
The goals of using medications are to start or keep up remission (no symptoms) and to improve quality of life. Each person reacts a little bit differently to each drug and many need a combination of drugs. While some of them have side effects, the benefits and symptom relief often outweigh those drawbacks. Learn more about each class of drug in the Living with IBD pages.
Aminosalicylates help control inflammation, especially in those who are newly diagnosed with mild symptoms.
Sometimes these drugs are called 5-ASA’s, which stands for 5-aminosalyciclic acid.
Examples include: Balsalazide. Mesalamine. Olsalazine. Sulfasalazine.
Possible side effects include: belly pain, diarrhea (loose stool), headaches, heartburn, nausea and throwing up.
These drugs can be very helpful right away. They help lessen inflammation quickly.
These are often given in large doses when the disease is at its worst, then lowered as symptoms get under control. They are given to people with moderate to severe symptoms.
These drugs are not given for long-term use.
Examples include: Prednisone. Budesonide. Hydrocortisone. Methylprednisolone.
Possible side effects include: Weight gain, acne, facial hair, mood swings, bone mass loss, greater risk of infection, hypertension and high blood sugar (diabetes).
Stopping these drugs suddenly could cause withdrawal symptoms, so your doctor will have you lower the dose slowly.
Immunosuppressants block the immune reaction that leads to inflammation, lessening swelling in the gastrointestinal (GI) tract.
These drugs can take up to three months to start working, so they are often used with other medicines until that time.
These are given to help people go into remission or given to people who have not responded to other treatments.
Examples include: 6-mercaptopurine (6-MP). Methotrexate. Azathioprine. Tofacitinib.
Possible side effects include: nausea or throwing up, diarrhea (loose stool), less able to fight infections (from low white blood cell count), fatigue or feeling tired, and pancreatitis.
These drugs can lessen inflammation and quickly bring on remission of ulcerative colitis.
They are used in people with moderate to severe ulcerative colitis who do not respond to other treatments.
These drugs are often given by either injection or infusion every six to eight weeks, based on what the patient needs.
They tend to cost more, so talk to your health plan before starting.
Examples include (brand names may be different):
- Tumor necrosis factor (TNF) antagonists (infliximab, adalimumab, certolizumab, natalizumab).
- Integrin receptor antagonists (vedolizumab).
- Interleukin (IL) 12 and IL-23 antagonists (ustekinumab).
Possible side effects include: Toxic/allergic reaction, itching or bruising at injection or infusion site, greater chance of getting infections (especially tuberculosis), and greater chance of lymphoma.
Biosimilars have been approved by the U.S. Food and Drug Administration (FDA) to use as treatment in place of existing biologic drugs.
They are based on an existing (originator) biologic but are not an exact copy.
Biosimilars work the same way as their originator biologics and are given the same way. Read more about biologics and biosimilars.
Your doctor can prescribe a biosimilar as a substitute for a biologic drug; however, your pharmacist cannot change you from a biologic drug to a biosimilar without your doctor’s approval.
Other medications
- Acetaminophen can be used for mild pain.
- People with ulcerative colitis should not take ibuprofen, aspirin or naproxen as they can make symptoms worse or cause GI bleeding.
- Antibiotics are given to prevent or treat infections and fistulas (a link between two body parts that should not be there, such as between two organs; they can form from infection, inflammation or surgery).
- Loperamide is given to help slow or stop severe diarrhea. It should only be taken for short cycles of time.
Surgery for ulcerative colitis
Even with the availability of medicines to treat ulcerative colitis, surgery may still be needed to manage the disease. There are a few types of surgery that your gastroenterologist with discuss with you.
Proctocolectomy
Removes the colon and rectum. Sometimes ileostomy is also done at this time, which is a procedure that brings the ileum, or end of the small intestine, through an opening in the abdominal wall to allow intestinal waste to drain out of the body. After the procedure, the patient wears an external bag over the opening to collect waste.
Restorative proctocolectomy (also known as ileoanal pouch anal anastomosis)
Removes the colon and rectum but allows the patient to continue to pass stool through the anus.
Before having surgery for ulcerative colitis, it is important to understand what the aim of the surgery is, what will happen during the procedure and the length of the recovery period. Patients with ulcerative colitis having surgery should speak to other patients who have had the procedure. Previous patients are often very willing to share their experiences and add perspective.
Newly diagnosed with ulcerative colitis
No matter what you may be feeling upon hearing you have ulcerative colitis, it is of great value to know that you are not alone. Many places have support groups, both in-person and online, for people all ages that can be very helpful. Talk to your health care provider about support groups at their office or the hospital or do your own research to get involved with the ulcerative colitis (and IBD) community.
If you are overwhelmed by your new diagnosis, don’t wait to reach out to a mental health expert to talk through the changes. Relaxation techniques, such as yoga, meditation or mindfulness, may be very helpful.
Working together with your health care team, you can make a treatment plan just for you, to help control your symptoms and put you in charge of your ulcerative colitis.
Questions to ask your health care provider
- How often do I need to see a gastroenterologist?
- How often do I need to undergo testing?
- What are my risks for colon cancer?
- Are there symptoms that should cause worry? If so, what are they?
If you don’t know something at any point, ask for more (or clearer) information! For some, hearing that they have ulcerative colitis is a relief, a reason for symptoms and a light at the end of the tunnel. For others, it can be scary and daunting. Many will have a mix of feelings. All of this is completely normal.
Complications of ulcerative colitis
Taking your medicine and staying well hydrated and nourished can help keep ulcerative colitis under control. Sometimes, though, complications can happen. Often, with ulcerative colitis, these issues will need medical attention.
Ulcers in the intestinal lining can open and bleed. Bleeding can cause anemia, which can be treated with diet changes and iron supplements. If you have a large amount of bleeding in your intestine over a short period of time, you may require surgery to stop the bleeding.
Severe bleeding is a rare complication of ulcerative colitis.
This happens when the large intestine is unable to absorb fluids and nutrients because of diarrhea and inflammation.
You might need intravenous (IV, into your vein) fluids to replace lost nutrients and fluids.
Some corticosteroid medications taken to treat ulcerative colitis symptoms can cause:
- Osteoporosis — the loss of bone
- Osteopenia — low bone density
Your health care providers will monitor your for bone loss and can recommend calcium and vitamin D supplements and medications to help prevent or slow bone loss.
Your immune system can trigger inflammation in your: joints, eyes, skin or liver.
Your health care provider can treat inflammation by adjusting medications or prescribing new medications.
This is a serious complication that occurs when inflammation spreads to the deep tissue layers of the large intestine. The large intestine swells and stops working. It can be a life-threatening complication and most often requires surgery.
Megacolon is a rare complication of ulcerative colitis.
If you think you are having one of these complications of ulcerative colitis, let your doctor know right away.



